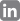AOE’s monthly newsletter that offers accreditation board bulletins for the ACCME, ACPE, and ANCC, along with updates on the Physician Payments Sunshine Act, highlights of AOE services, and information on upcoming activities and educational opportunities.
AOE Compliance Connection – July 2025 Newsletter
Welcome to the July edition of AOE’s Monthly Newsletter! This edition of AOE Compliance Connection includes insights from the ACCME 2024 Annual Data Report, the fourth installment of our series about Initial Accreditation, and an update on exciting developments at AOE. In addition to our monthly newsletter, check out AOE’s weekly compliance tips for quick, applicable advice your team can use for compliance success.

ACCME: 2024 Annual Data Report Results
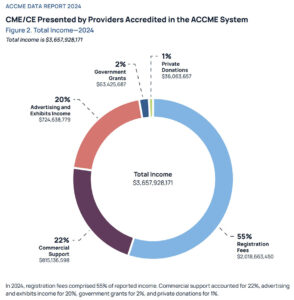
The ACCME released its 2024 Annual Data Report on July 1, 2025. The report analyzed data from 1,561 accredited providers who offered, collectively, 250,325 activities last year. Whether you’re a seasoned member of the CME/CE workforce or new to the enterprise, it’s worth reading for a current state of affairs (click here for the full report).
Here are a few findings we found particularly noteworthy:
Record High Income: In 2024, Total Reported Income across the ACCME system reached an all-time high of $3.7 billion. This is a testament to the upward trajectory of the CME/CE enterprise, which continues to grow both interest and investment from various stakeholders.
Funding Diversification: While commercial support was down (a 5% year-over-year decline), it still comprised 22% or $815 million of total income. A significant portion of reported income came from registration revenue (55% or $2 billion) and advertising and exhibit income (20% or $725 million). As providers contend with industry changes including provider consolidations, diminished, traditional funding sources like government grants and private donations, looming budget cuts, and so forth, they can continue to diversify their funding methods. There is an air of possibility here for accredited providers of all sizes.
Activity Types: Popular educational activity formats included Enduring Materials (46% of all activities), Live Conferences (over 40% of all activities), and Regularly Scheduled Series (11% of all activities). To echo ACCME President and CEO Graham McMahon, each of these pose “a distinct and complementary role in supporting clinician learning,” which is why many of our provider clients continue to see success with these formats.
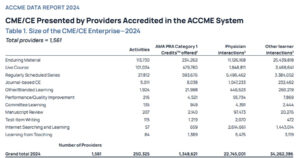
CME/CE Learning Outcomes: Per the report, more CME/CE activities are now evaluating Learner Competence (95%), Learner Performance (46%) and Patient Health (18%). While these activity outcomes still skew more subjectively (e.g., self-reported changes) than objectively (e.g., observed or tested changes), this upward trend shows that providers are dedicated to generating real changes in clinical practice and outcomes.

Initial Accreditation Series, Part 4: Self-Study
Interested in applying for Initial Accreditation with the ACCME? Last month, we provided an overview of ACCME’s Pre-Application Review Process and details for each step.
This month, we focus on a critical “storytelling” component of your Initial Accreditation application—the Self-Study Report (SSR).
In basic terms, ACCME’s Self-Study Report is an opportunity for you to tell the ACCME what your CME program mission is, demonstrate how you’re achieving that mission, and prove your achievement is in accordance with ACCME’s Criteria, Standards for Integrity and Independence, and policies. Think of it as a long, hard look in the mirror, a revealing peek into your program’s goals and the extent to which you are truly (and compliantly) realizing them.
While this might seem like a daunting task, the ACCME provides instructions on what to include in your Self-Study Report, so you know exactly what to address.
Here’s what to expect, along with our recommendations to help you get started:
ACCME’s Self-Study Report outline will include specific questions you’ll need to answer. ACCME’s Program and Activity Reporting System (PARS) includes a Self-Study Report section with specific questions about your program (e.g., history, organizational structure, mission statement, expected results, and more). Be sure to note the answer field requirements (e.g., word count limits, etc.) as you compile your responses.
You’ll be asked to provide descriptions, attachments, and examples related to your CME Program. Per the ACCME, “Descriptions are narrative explanations. Attachments are specific documents. Examples are demonstrations of the implementation of the practices described that may include narrative and/or attachments.” These required materials give you the opportunity to “prove” your CME practice(s) align with ACCME’s Accreditation Criteria, Standards for Integrity and Independence, and applicable policies.
You have one primary contact but consider your full team. Because your report is a comprehensive narrative that covers your entire CME program, think about the full team involved. Consider who should be consulted in which capacities, and how they can contribute their input to your report. ACCME corresponds with ONE primary contact at your organization for all accreditation purposes, but the actual drafting process might involve several parties! Please reach out to AOE for any assistance you might need in the management and/or review of the SSR and accreditation process.
ACCME may contact you after submission. Before you submit your Self-Study Report and any supporting materials in PARS, make sure you’ve thoroughly addressed the ACCME’s questions. If your report is incomplete or the ACCME has follow-up questions, they will contact you.
Organization and timelines are critical. When mapping and timelining your process to complete your Self-Study Report, there’s several factors to consider—including your approval of eligibility and the next available cohort. This tends to be a more challenging element of the process. If your team is interested in assistance or management on this front, reach out to the AOE team here.

CE/AOE Community: A Busy Summer at AOE
AI Update: Like many professionals in the accredited CME/CE enterprise, AOE is identifying new ways to deploy AI tools to help accredited providers save time and cost in managing activities. Specifically, AOE is evaluating tools to streamline and cross-reference faculty disclosures, content, and a proprietary data set of validated content and terminology that will allow users to rapidly assess and approve accredited CME/CE materials. We look forward to sharing these results and potential tools this year!
AOE Team: We’re gearing up for two industry events next month. AOE Program Manager Chantel Crowl will represent the AOE team at the Colorado Alliance for Continuing Medical Education (CACME) 2025 Annual Leadership Conference in Aurora, CO on August 15th. In addition, we are finalizing our list of staff who will represent our team at the ACCME 2025 Accreditation Workshop in Chicago, IL on August 26th and 27th. Interested in attending/want more details? Visit CACME here and ACCME here.
Upcoming Events
- AAMSE Annual Conference
July 16-18, 2025, Chicago, IL
Read More >> - ACPE Self-Study Workshop
July 23-24, 2-25, Chicago, IL
Read More >> - Newcomers’ Orientation to Accredited CE
August 25, 2025, Chicago, IL
Read More >> - ACCME 2025 Accreditation Workshop
August 26-27, 2025, Chicago, IL
Read More >>